
Laboratory Investigations in Microbiology

 |
Laboratory Investigations in Microbiology |
 |
Medical microbiology concerns itself with the etiology of disease, the isolation and identification of pathogens, and the appropriate treatment regimen. In the last exercise we cultured microorganisms from the throat, skin, and enteric tract. Although the microbes we cultured were normal (resident) to the human body, they may very well have included pathogens. Should an infection be present, similar culture methods would be used to isolated potential pathogens, such as Staphylococcus aureus (wounds), Pseudomonas aeruginosa (wounds), Enterococcus faecalis (cardiac infections), Bacillus cereus (intestinal tract infection), E. coli (intestinal tract), or Salmonella (intestinal tract). Once identified, the correct treatment method must be selected. Can any antibiotic be used? Which antibiotics are most effective? Which are most appropriate?
Choosing the proper antibiotic is important for several reasons. 1) Some
bacteria are naturally insensitive to certain antibiotics; 2) Some bacteria
are resistant to antibiotics (e.g. MRSA and 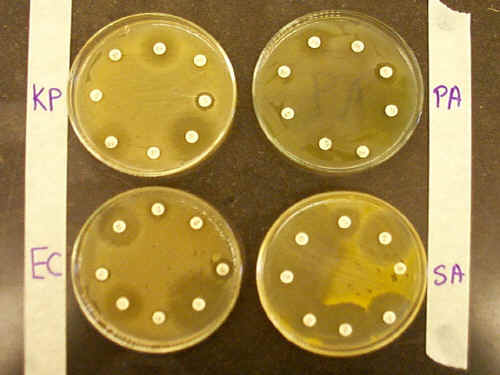 VRE);
3) A broad-spectrum antibiotic often wipes out beneficial bacteria - a
narrow-spectrum antibiotic is preferred; 4) You want to select the antibiotic
that is most effective with the fewest side effects; 5) Some patients are
allergic to the first-choice antibiotic and secondary antibiotics need to be
identified that still work.
VRE);
3) A broad-spectrum antibiotic often wipes out beneficial bacteria - a
narrow-spectrum antibiotic is preferred; 4) You want to select the antibiotic
that is most effective with the fewest side effects; 5) Some patients are
allergic to the first-choice antibiotic and secondary antibiotics need to be
identified that still work.
The traditional method for identifying the effectiveness of an antibiotic is called the Kirby-Bauer method. This involves swabbing the bacteria onto an agar plate (to form a bacterial lawn) and placing antibiotic-impregnated disks onto the agar surface. After incubation, bacteria will grow everywhere on the plate except near the antibiotics they are sensitive to. By measuring the diameter (in millimeters) of each Zone of Inhibition, one can determine the effectiveness of each antibiotic. The measured zone is compared to a table of critical values for each antibiotic. If the zone diameter is less than the critical value for sensitivity, it may be resistant (natural or acquired) to that antibiotic.
4 CULTURE BROTHS (E. coli, P. aeruginosa, K. pneumoniae, S. aureus)
4 Sterile cotton swabs
4 Mueller Hinton agar plates
Antibiotic disk dispenser (to share)
Thursday
© 2003 - 2022 José de Ondarza, Ph.D.