- Elephantiasis (Filariasis) - obstruction of lymphatics
- Acute-phase response to LPS: sepsis
- Inflammation: Lyme disease
- Antibody cross-reaction: rheumatic fever
- Granuloma formation: tuberculosis
- Viral infection: cytokine release
- Fermentation products
- Acid & Gas: Gas gangrene (C. perfringens)
- Enzymes
- Phospholipase C (alpha toxin)
- collagenase
- hyaluronidase
- fibrinolysin
- lipase
- streptolysin
- DNAse
- protease
- LPS of Gram-negative bacteria
- Lysis releases LPS - activates cytokines
- IL-1, IL-6, TNF, prostaglandin
- fever, septic shock, capillary leakage, inflammation
- intravascular coagulation (DIC) & complement activation
- Heat sensitive proteins
- Highly toxic by themselves
- Secreted by bacteria; may enter circulation
- Cholera toxin: activates G-protein + adenylate cyclase
- Pertussis toxin: inactivates G-protein, activates adenylate cyclase
- Diphtheria toxin: inactivates EF-2, blocks protein synthesis
- Botulinum toxin: blocks exocytosis of acetylcholine
- Tetanus toxin: blocks release of inhibitory neurotransmitters
- Cytolysins (e.g. lecithinase) - gas gangrene
- Hemolysins: lyse red blood cells
- Anthrax toxins (EF, LF, PA) - cause edema, cell death
- Shiga toxin (Shigella dysenteriae) - inhibits protein synthesis
- Enterotoxins: LT, ST
- Activate T-cells without need for a specific antigen
- Release of IL-1 (fever) & IL-2, TNF (hypotension/shock), death of T-cell
- Example:
- Staphylococcus TSS toxin & enterotoxin;
- S. pyogenes erythrogenic toxins
- Cell lysis
- Inhibit cellular DNA synthesis & degrade host cell DNA (HSV)
- Inhibit host cell protein synthesis (polio, HSV, poxviridae)
- Cell membrane alterations (enveloped viruses)
- Cell fusion - syncytia formation (HSV, HIV, Paramyxoviridae)
- Inclusion bodies
- Negri bodies (Rabies)
- Owl's eye (CMV)
-
Cowdry
intranuclear inclusions (HSV)
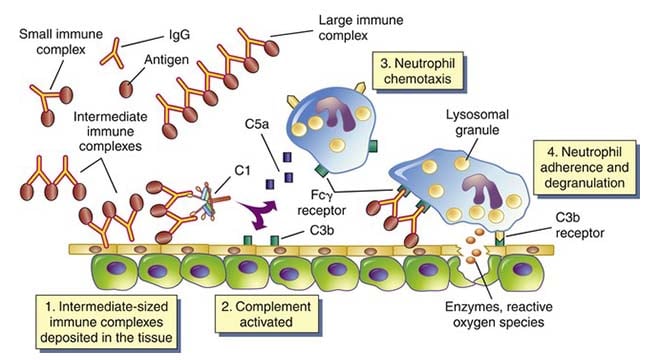
- Immunopathogenesis
- Cytokines & interferon: flu-like symptoms
- Type III hypersensitivity & inflammation: mumps, measles, hemorrhagic fevers
- Immune complex formation: rubella, HBV
- Latency: HSV
- Persistent infection: Many enveloped viruses
- Transformation - cancer (oncogenic viruses)
- activation of cellular genes (EBV)
- deactivation of cellular control signals s.a. p53 (HPV)
- inhibition of apoptosis (EBV)
- viral genes which activate growth (non-human retroviruses)
- insertion of viral DNA near growth-promoting human genes (HTLV)
- tissue damage that necessitates frequent cell division (HBV)
* Why do children exhibit less severe symptoms to mumps, measles and chickenpox than adults?
- Colonization of the host
- Immune system evasion or deficit
- Growth and/or dissemination
- Obstruction: blood vessels, lungs (Aspergillosis)
- Hydrolytic enzymes: proteinase, elastase, phospholipase
- Immunopathogenesis: inflammation (Ringworm), granuloma formation (mycetoma), immune complexes (Coccidiodomycosis), abscess (Candidiasis)
- Tissue damage: lesions, fibrosis, edema
- Hydrolytic enzymes: proteinase, elastase, collagenase
- Ionophores (Entamoeba)
- Endotoxins (Trypanosoma)
- Obstruction (Ascaris)
- Migration of larvae (flukes)
- Immunopathogenesis: inflammatory (Trypanosoma), immune complexes (Malaria)