Anthrax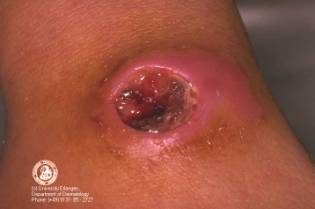
Introduction
Anthrax is a rare zoonotic disease often transmitted from contaminated soil
in cattle yards or from the hides of infected animals. The majority of cases are
cutaneous (a.k.a. Woolsorters disease), but when spores are ingested
(gastrointestinal) or inhaled (inhalational), a more serious systemic infection
occurs. Anthrax is of note because of its bioterrorism threat.
Summary
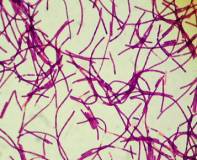
- Cause: Bacillus anthracis
- Microscopy: Gram-positive rods with spores
- Symptoms: Anthrax has 3 clinical forms: cutaneous,
gastrointestinal, and inhalational
- Cutaneous: painful papule develops into ulcer, then into a necrotic
eschar. Painful lymph node infection, fever and edema may develop
(systemic spread). Mortality is 20%
- Gastrointestinal: Ulcers in mouth and esophagus, or nausea, vomiting
and malaise (large intestine infection); ssytemic spread, sepsis, edema
and mortality near 100%
- Inhalational: Fever, shortness of breath, cough, headache, vomiting,
chills following a 0 - 2 month latency. Edema, fever, shock with near
90% mortality
- Transmission: Direct contact with animals or contaminated soils;
ingestion of contaminated meat; inhalation of spores
- Pathogenesis: B. anthracis can invade macrophages and remain hidden
there for a while. This usually spreads the bacteria to the lymph nodes. B.
anthracis produce exotoxins: Lethal Factor (stimulates TNF and cytokine release
from macrophage) and Edema Factor (stimulates adenylate cyclase,
causing edema).
- Treatment:Ciprofloxacin, pen, chloramphenicol, dox, erythromycin
- Prevention: vaccine